Recent drug discoveries promise new treatments and cures for many diseases. However, getting a drug to work, not only in experiments with cells in the lab, but also in the human body, is difficult. One challenge? Getting past the body’s line of defense, the immune system, which fights foreign invaders that make it into the body.
In September, a news article published in Nature reported that scientists have figured out an improved method to get drugs past the immune system. The process uses tiny, man-made carriers, called nanoparticles, covered in a cloak that makes them look like cells in your blood. With this cloak, the particles can evade attack and arrive at their intended destination, whether the destination is a site of bacterial infection or a broken blood vessel.
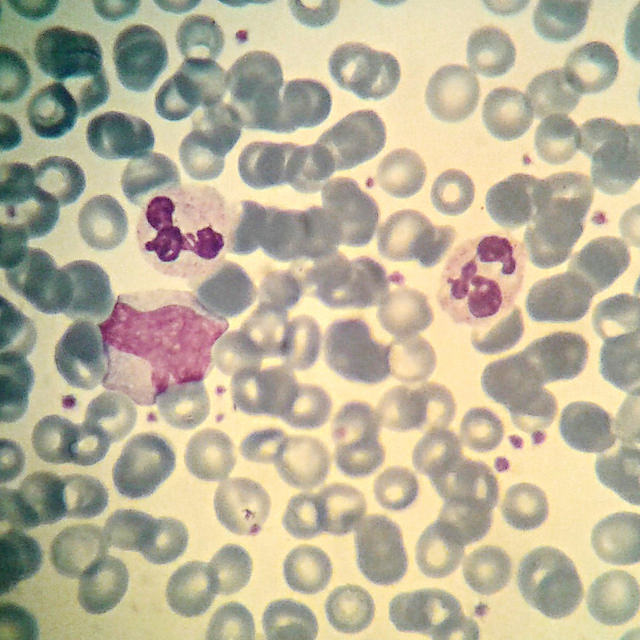
Cells in your blood, like those shown in this microscope image, are coated in membranes that the body recognizes as non-foreign, preventing the immune system from attacking them. Cloaking nanoparticles in such membranes allows them to slip past the defense system unnoticed, so they can deliver drugs to sites in the body without confrontation. (Hanna Sӧrensson, Flickr, Creative Commons)
Nanoparticles have been acknowledged as an option for drug delivery because they are small enough to enter the body and can be directed to specific sites, allowing for targeted treatment that requires lower doses of drugs and reduces harmful side effects. However, nanoparticles look foreign to the body, and often trigger the immune system to attack and divert the nanoparticle and its cargo of drugs from arriving where they need to be. While scientists have attempted to disguise nanoparticles by coating them with various proteins that tell the immune system not to attack, this newest research goes a step further by giving the nanoparticles a cover of membrane, completely outfitted with all of the proteins that cells, called platelets, already have. As the news report suggests, this is a major step forward in engineering new devices that are compatible with your tissues, making it possible to use man-made technology to treat human diseases.
However, a lot of research needs to be performed to determine how broadly applicable such membrane-coated nanoparticles will be in the clinic. While the research tested the ability of these particles to make it past the immune system and deliver antibiotics against one type of bacteria, MRSA, more experiments will need to be performed to see whether the same effect is seen with other types of bacterial infections, or if this technology might be used to treat viral infections. Additionally, one current limitation of these membrane-cloaked nanoparticles is that while some of them make it to the intended destination to perform their jobs, a large number of them end up disposed of in the body’s liver and spleen. Further research into increasing the efficiency with which the particles are delivered to the intended destination, such as by enhancing the cloaking process, will improve how many of the nanoparticles make it to the intended destination, rather than being diverted by the immune system. Lastly, the use of membranes promises flexibility in nanoparticle bioengineering. Scientists may be able to insert different sets of proteins into the membranes to specifically direct the path or function of the particle in various scenarios, further broadening the use of this technology.
By Emily Low, Harvard University
Acknowledgments: Special thanks to Jernej Turnsek, a graduate student in the Biological and Biomedical Sciences program at Harvard Medical School, for expert advice on bioengineering and nanoparticles.
Featured image courtesy: BiotechGuru












Why does nanoparticle target a specific desired site?