Researchers from the Netherlands have found a way to “grow” artificial mouse blastocysts by combining different stem cells in a dish. The artificial embryos resemble natural ones so closely that, when transferred into a mouse’s uterus, they initiate pregnancy. They can easily be mass-produced and could serve as new models for drug development, possibly leading to infertility treatments and early interventions for other diseases.
At the moment doctors have no idea how to intervene if problems come up in the earliest stages of pregnancy. Consequently, pregnancy might not come to term, or the baby might develop health problems later in life. Researchers from Maastricht University and the Royal Netherlands Academy of Arts and Sciences created the “study” model for the early stage of pregnancy and published their findings in Nature.
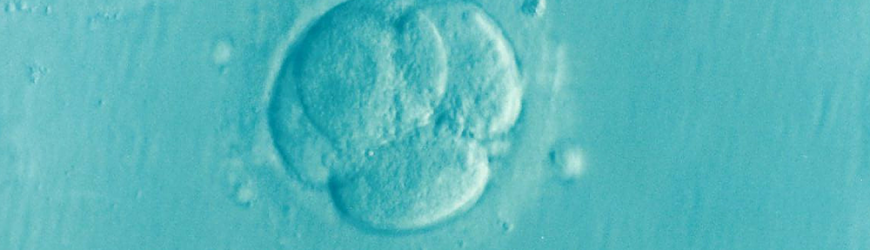
Why research blastocysts? For one, they contain all the stem cells that are going to form the whole embryo and placenta. These hollow spheres are made of fewer than 100 cells that form within days after an egg is fertilized, and are not yet implanted in the uterus. Once implanted, the cells within the blastocyst (inner cells or embryonic cells) become the embryo while the cells forming the sphere (outer cells or trophoblast cells) become the placenta.
“Other labs have previously shown that stem cell lines representing these inner and outer parts can be cultured independently and multiplied in the laboratory,” Nicolas Rivron, lead researcher on the Dutch study, said to Research Gate. “By combining these mouse stem cells, we have now succeeded in creating embryo structures in the laboratory.”
Other research groups have successfully created models from later stages in an embryo’s development – post-implantation models called “gastruloids”. Rivron’s group is the first to produce a pre-implantation artificial embryo with placenta-forming cells, trophoblasts. To create their model, a “blastoid” – collection of first embryonic and trophoblast mice stem cells, were grown separately in the lab. Afterward, they were combined at a specific ratio and stimulated with a cocktail of molecules. That initiated their communication and triggered them to self-organize.
“The artificial embryos are so similar to natural embryos that they nest successfully in the womb and start a pregnancy,” said Rivron.
After the artificial embryo was transferred to a mouse’s uterus, it got implanted just like a natural one would during pregnancy. The cells divided further and the trophoblast cells fused with the mother’s blood vessels and established the first connection that supplied the embryo with the mother’s blood.
Because researchers can create blastoids from stem cells in large numbers, they can finally start to uncover the secrets behind this crucial stage of development.
“For the first time, we can study these phenomena in great detail and run drug screens to find medicines that could prevent infertility, find better contraceptives, or limit the appearance of epigenetic marks that appear in the blastocyst and lead to diseases during adult life,” said Rivron.
In humans, a blastocyst forms just five days after fertilization and this stage can influence the success of a pregnancy and the resulting baby’s health post-birth. So far, it is unclear if a human uterus would respond to these blastoids in the same way. Researchers agree that discoveries such as this one could help everyone: the mother, the fetus, and the baby it develops into.
Watch the interview with Nicolas Rivron and learn more about his research:
To learn more about first successfully transplanted reprogrammed stem cells in humans,
watch the video below:
By Andreja Gregoric, MSc